What is "Normal" in Grief?
/ Understanding Grief : Eleanor Haley
For further articles on these topics:
Here's a test question for you:
Which of the following grief related behaviors is abnormal?
A. A father who visits his son's grave every morning
B. A widower who continues to wear his wedding ring 5 years after his wife's death
C. A woman who refuses to part with her deceased mother's belongings
D. A woman who avoids the restaurant where she met her deceased husband
E. A man who experiences intensely emotional days two years after his daughter's death
F. None of the above - you have no idea what's normal for anyone else in their grief.
If you guessed (F), congratulations you get 100%.
"Am I normal?" and "Is this normal?"are questions commonly asked by grieving people.
When faced with complex and overwhelming problems, humans are hardwired to simplify by looking for patterns, rules, and categories. So we push, shove, and sort the wide and variable experience of grief into neat little boxes, and when we're finally finished we step back and say "Okay! Now we can deal with this situation."
Simplifying and categorizing the world may be helpful in a number of scenarios, but it can lead us woefully astray in grief. From person-to-person, situation-to-situation, and culture-to-culture there is such immense variation in grief reactions, emotions, thoughts, and behaviors. Grief depends on the bereaved, their relationship to the deceased, secondary stressors, coping style, support system, and the list goes on. So, it's difficult to define "normal."
Grief reactions typically exist for a reason. In the beginning, one may feel intense yearning, pain, sadness, loneliness, anger, guilt, etc. As traumatic as all this may feel, these thoughts and emotions are reinforced by virtue of the fact that they (1) allow a person to stay connected to their loved one and (2) are enduring proof of the significance of the death. As time goes on (and remember, there are no specific timelines to grief), grief related thoughts, emotions, and behaviors continue to to be useful in maintaining an ongoing bond with the person who has died, constructing a narrative around the loss, and, in some cases, as a necessary part of experiencing posttraumatic growth.
Interestingly (and confusingly), the intensity of emotion and the content of thoughts may change, even though someone's overt behavior may not. This is another reason why the delineation of 'normal' vs 'abnormal' is so impossible in grief, because your relationship with certain thoughts, objects, and emotions changes over time. So where one day (sad + crying) = intense distress, another day (sad + crying) = feelings of closeness to the deceased.
This is why I think a more appropriate question to ask yourself, albeit one that feels a little glib, is...
"How is this working out for me?"
The "How's that working out for you?" question is sarcastic and snarky and so it’s a shame I find myself using it all the ever-loving time. I’m sorry, but it just seems to apply in many mental health situations. Unlike physical health where illness and injury are often objective (an untreated broken bone will almost always get in the way of one’s daily functioning.), mental wellbeing is often determined by a person’s subjective experience.
I think this question is especially relevant where grief is concerned because things that look like an expression of pain, erraticism, or impulsivity to the outside observer – like minor acts of avoidance, holding onto items, sudden shifts in perspective, making major life decisions, and continuing to mourn for years into the future – may actually be positive, comforting, and adaptive to the individual.
When it comes to grief reactions, instead of asking if the behavior reflects what is "normal" or "expected" perhaps one should instead ask…
- “What was the impetus for this feeling or reaction?”
- “Does this feeling or reaction make sense when you consider the context?”
- “Did the bereaved experience this feeling or reaction as distressing?”
- “Does this behavior help the bereaved cope with their grief?”
- “Does this behavior help the bereaved maintain connection with their loved one?”
- "Is this feeling or reaction harmful or dangerous?"
- And finally, “Are these feelings and/or grief reactions standing in the way of the bereaved living a life that is consistent with their values as an individual, family member and friend, or as a member of society?”
So, not in so many words, “How's that working out for you?”, and if the overall answer to this question is "not well" then it might be time to change course.
Now I realize that by insisting there are no rules to grief, I've made the idea of identifying "problems" and "changing course" exponentially more difficult. Without black and white - normal vs. abnormal - rules, how are you supposed to know when you've subtly crossed the threshold into troubling territory? Sorry, all I can say is this:
First and foremost, one thing that is always black and white is that if you've been having thoughts of harming yourself or someone else, it's time to talk to someone right away.
- Call the National Suicide Prevention Lifeline at 1(800)-273-TALK
- Call 911
- Go to the nearest emergency room
- If possible, speak with your therapist
Beyond that...
If you're uncomfortable.
If you believe you need a little help or guidance.
If you feel your experiences go beyond what is typical for you.
If you're experiencing elevated, ongoing, and unrelenting distress (anxiety, hyperarousal, intrusive thoughts, etc).
If you're experiencing ongoing and unrelenting depressed mood (lack of interest in activities, hopelessness, decreased energy, etc).
If you feel stuck in your grief and you aren't sure what to do next.
Then it wouldn't hurt to seek a little extra help via a therapist, support group, workshop, education, etc.
And of course, continue to visit What's Your Grief by subscribing to receive posts straight to your email inbox.
We wrote a book!
After writing online articles for What’s Your Grief
for over a decade, we finally wrote a tangible,
real-life book!
What’s Your Grief? Lists to Help you Through Any Loss is for people experiencing any type of loss. This book discusses some of the most common grief experiences and breaks down psychological concepts to help you understand your thoughts and emotions. It also shares useful coping tools, and helps the reader reflect on their unique relationship with grief and loss.
You can find What’s Your Grief? Lists to Help you Through Any Loss wherever you buy books:





Judy May 2, 2021 at 3:45 pm
My youngest daughter 51, died 3 years ago of a quick, deadly cancer. I was very close to her. I am still going through the grieving process. I was denied being able to spend meaningful time with her during the last few months of her horrible death. Her partner wouldn’t let me be with her. I wasn’t there when she died and she wanted to be cremated so I have no place to visit her now. We planted a beautiful tree that summer, in her honor. I can sit and watch it change & grow with the seasons. She loved Spring, gardening and life. Her birthday was in May and the beautiful blossoms remind me of what a beautiful, person she was. I have an especially hard time in the Spring. I miss her so much! I don’t know whether my grief is normal after three years or if I have PTSD. connected to her death.
Lowell April 23, 2021 at 10:39 pm
My bride died four years ago after 35 years together. 29 years of recurring brain tumors, a final year of medical mudslide, and two months in home hospice. The day her oncologist broke the news that they had run out of any viable treatment options, estimated she had about two months left, and suggested hospice, she didn’t bat an eye. She didn’t want to talk in the car on the way home. When I rolled her into the house and lifted her into the recliner in the den, she asked what I heard. I repeated what the doctor said, and she calmly said that’s what she heard too. She said, “I thought I had more time, but I know where I’m going. It’s OK.” She then gave me a six-point “honey-do” list. The first four items were about her final arrangements, and the fifth not to give up on a career aspiration. The sixth was that she wanted to match me up with one of her best friends, a dear lady with more baggage than an airline. For the next two days I told her “no handoffs.” When she persisted, I told her to think back 35 years to when I picked her up at the beach. I would figure that out when ready and it would take time.
She passed two months later with infinite grace and dignity. Two days before she died, she recalled it was our daughter’s 4th wedding anniversary and she didn’t want to die on her anniversary.
After the kids left town, I went on a 10-day “trail of tears” basckpacking trip to process memories and shed my tears in wilderness solitude. I spent much of that time wailing my grief in the woods. Then I came home to go through her clothes for donation per her explicit directions. I wept over so many of her things that prompted bittersweet memories.
For the next three years I drowned myself in work and did a lot of financial catch-up, reading the point I could comfortably retire. I felt she was looking out for me.
At almost the two year mark, I went with a church group to Israel. At an overlook in the desert, the pastor remarked that we are not meant to linger in the valley of the shadow of death, but should move on through to the other side. Recognizing that I had been in that valley since her first diagnosis in 1988, I wept.
Returning home, I started clearing my basement and mentioned to a neighbor walking her dog that I though I might get the house ready to sell that year. The neighbor walked up the street to where another neighbor was hosting an elegantly staged realtor’s open house. Someone coming out of that house asked if anyone else in the neighborhood was thinking about selling but was not yet listed. Within 15 minutes, I had a buyer on my doorstep who made a fair “as is” offer. I had an estate sale, donated a truckload of stuff to Salvation Army, and by the second anniversary of my wife’s death had moved to a 1 BR high rise apartment as an interim step. Now I’m preparing to close on purchase of a nice townhome in a great location.
Knowing my wife’s demand that I find someone new, after a year I tried online dating for the first time. I wasn’t ready, and went back to Giefshare at church. I got a lot of dates, some with attractive, intelligent, pleasant women, but no one who seemed like a potential soulmate. Probably at least a dozen times, I’ve sworn off online dating, then went back to it after a couple of months of sitting home alone every weekend. The few friends who tried to set me up with single women completely misfired; none of the women they tried to math me with were anywhere near right for me.
Almost three years after my wife died, my college girlfriend to whom I proposed on my 21st birthday lost her husband after his long battle with cancer. I sent an appropriate condolence letter and maintained light contact on social media. After a year, I reached out, suggesting it might be time to get reacquainted and perhaps have lunch. She responded that she was still far too deep in her grief to even do that in the foreseeable future. That door seems irrevocably closed.
I often imagine getting to heaven, meeting my wife again, and her giving me a little side kick to the butt like she used to do, saying, “I told you to find someone else to love! Why didn’t you?”
So here I am, four years after my wife died, turning 70, lonely as hell, and totally burned out on the entire online dating scene. EHarmony, Match, Bumble, etc., have proven to be mostly a huge time sink. It reminds me of trying to find a key employee through Indeed.com, where one is inundated with hundreds of resumes from applicants who do not fit any of the essential qualifications. I’ve had one pleasant transitional relationship with a bright, attractive woman who was always clearly on a diverging trajectory. We had fun but clearly neither of us saw it as long term. Most of the women I’ve met in natural settings pre-Covid have been in my children’s generation. While women I meet naturally often guess my age 10-15 years low, I’m not meeting any age-appropriate prospects naturally, particularly during Covid. Online, my age number is emblazoned across the top of my profile and absolutely deters most women who are not elderly. I’m way too healthy and active for anyone I’ve connected with in the Silver Singles and OurTime sites.
There are several stages of recovery from loss of a spouse. I did a good job of addressing the first stages by sort of ripping off the bandaid. I quickly addressed the painful, bittersweet memories and forced myself to process grief. I went through the mental process of reassigning my wife to past tense and incorporating our love and my loss into my character. I avoided the three common traps for widower of selling the house too soon, making stupid financial decisions, or committing too soon to a rebound relationship. Then I unloaded the house and most of the stuff.
I’ve tried to move forward to a new relationship that would respect the great love my wife and I had for so long, consistent with her dying wish that I find someone new to love. I’ve gone through thousands of online dating profiles and had “meet and greet” first dates with probably 100+ women.
But at four years I’m stuck, still unable to find an appropriately bright, witty, energetic, age-apprropriate, with shared interests, sense of humor and chemistry. That is the last stage of processing grief and going forward to embrace life with love and joy as my wife demanded that the kids and I must do. I don’t hold my late wife on a pedestal, idealized in death beyond what she was in life. But I really want to find someone I can love and trust as much as I did her. Anything less would not honor what we had for 35 years.
How does one get past this impasse?
Rita bruneski December 11, 2018 at 8:10 pm
Wow lost my only brother ,sibling 21years ago glad for the memories this time of year watch my parents age but it does get better It really does it always will hurt he left behind three babes the youngest was 3 months old and a wife it gets real lonely grab your friends get some hugs and IT WILL GET BETTER RITA B
Denise June 15, 2018 at 10:33 pm
I guess I am new to this grief thing. Mom died the day after mothers day. She has had health problems for years but no one was expecting the brain bleed that happened that weekend. Her and dad had been married just shy of 58 years. He was devastated. But now I don’t know. I know he is grieving but we aren’t talking about it. And I don’t want to depress him more. I am the youngest of 3. Now, we are dealing with new developments in dads health. He is to have a kidney biopsy next week. The thing I am struggling with is a lack of confidence. It is like I am afraid of not being included with my family. This does not make a lot of sense as nothing had really been said and I talk to dad most every day. It is like I am suddenly a little girl who is terrified she won’t please her daddy. And I know my dad loves me. He is a great man. I expected sadness. Guilt. Anger even. But this is crazy. My husband has been great. I am just confused. And struggling.
Gloria June 15, 2019 at 12:22 am
Sorry for your loss. I hope you are doing better.
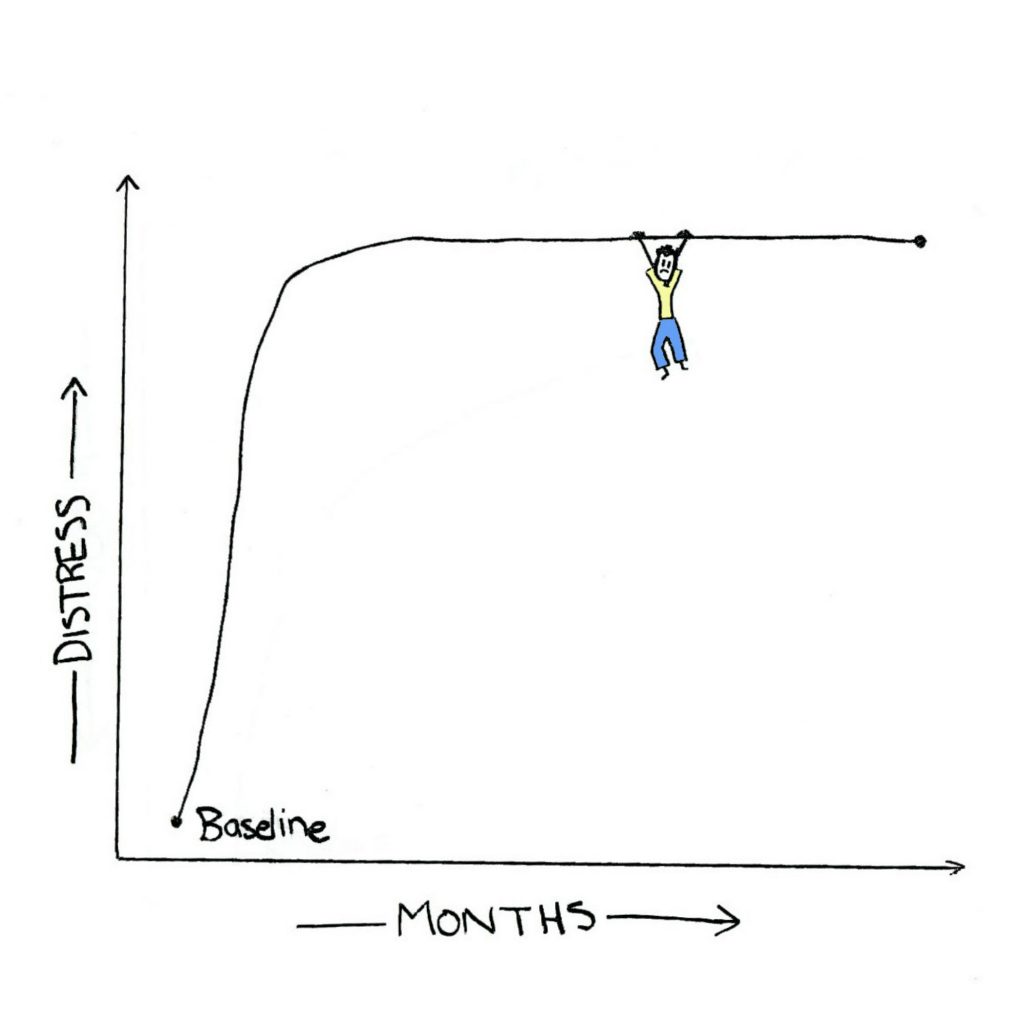
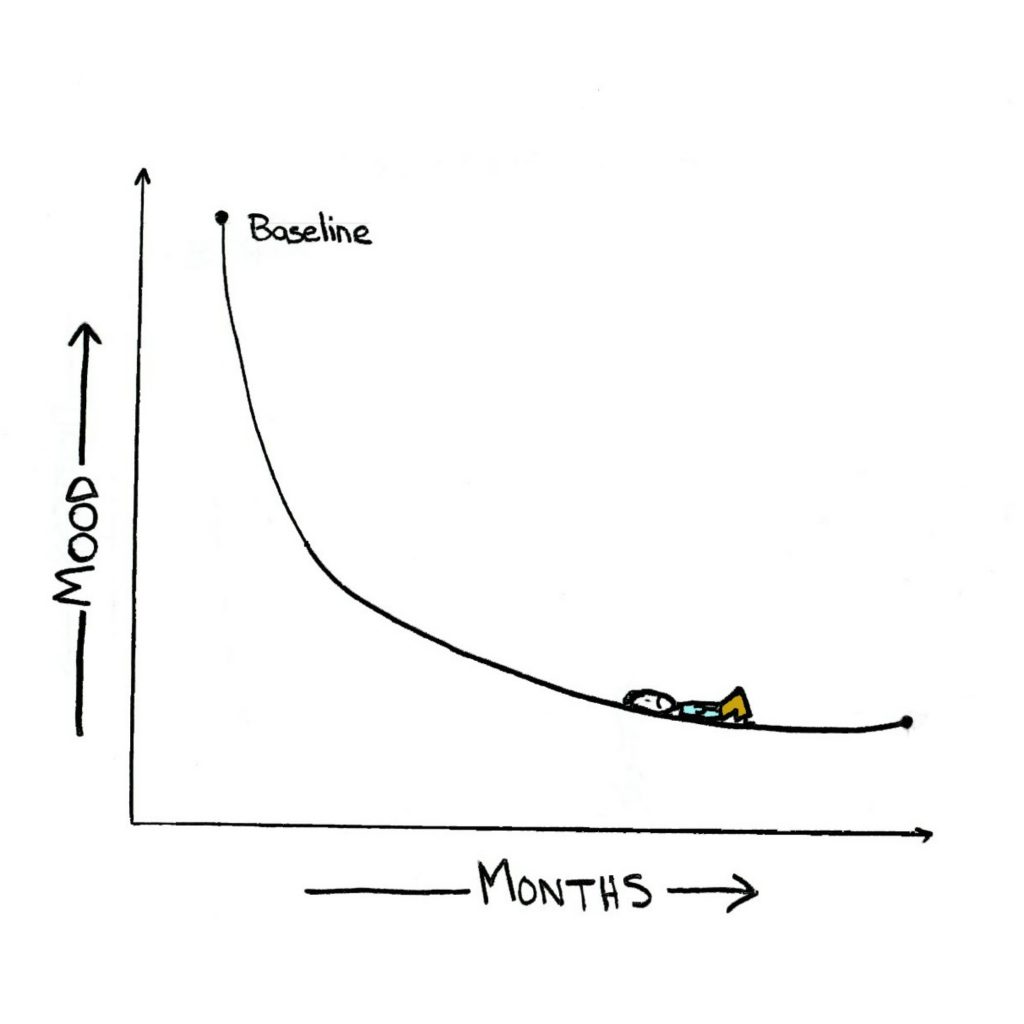
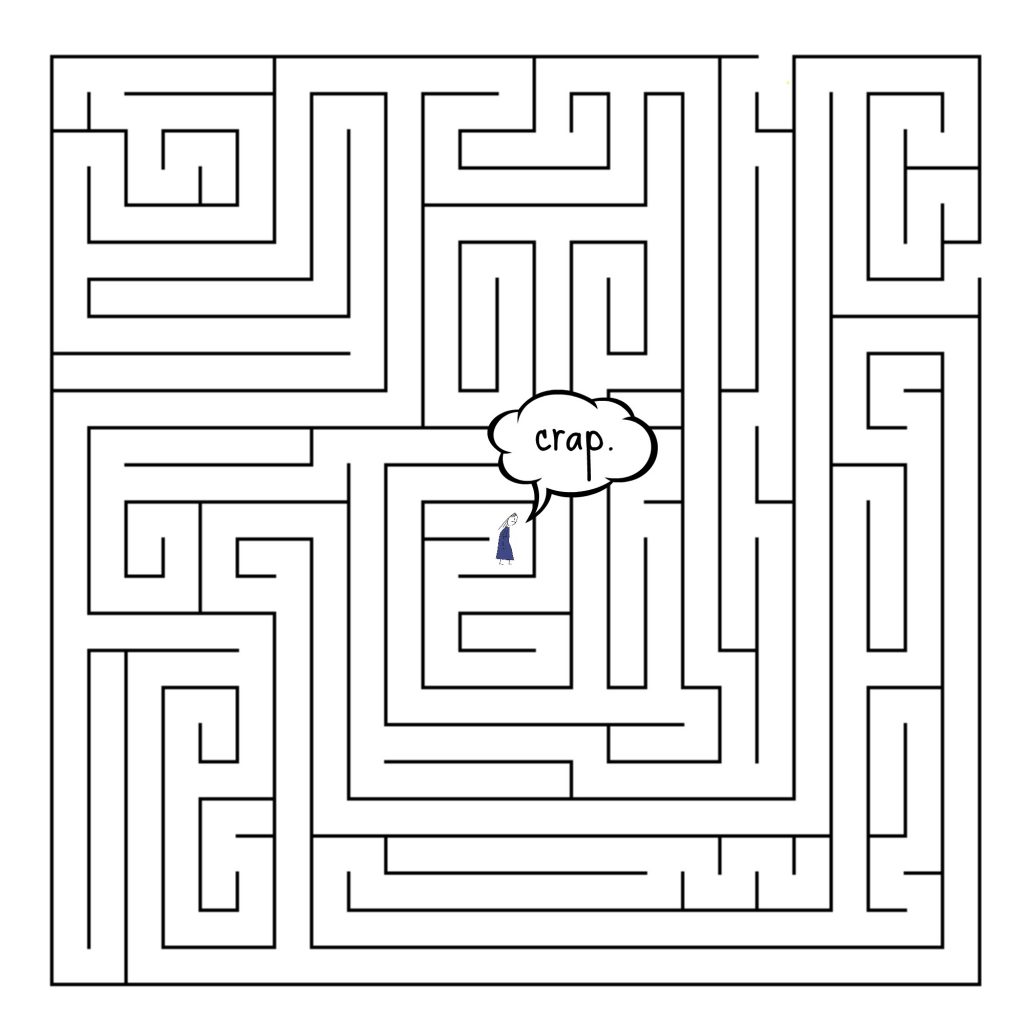
Steve March 29, 2018 at 1:45 pm
This is a good article, and I love the visuals, too. I was lost in the maze for a while, and then progressed to the downward slide. The most important thing in my nonprofessional opinion, but one whom has lost a wife of 44 years of marriage, is that you make some progress even if it is extremely slow. I have had a few serious injuries and a couple of surgeries over the years, and sometimes it was over a year to get over a physical injury. My father died in bed (completely unexpected as he was not ill) when I was 17. I know it impacted my life for the next decade or more. My wife died expectantly in bed, but she had been on dialysis for a few years. Sometimes, I ask God if He is trying to drive me crazy. This was kind of cruel. Early in the morning I have to get up from the bed and go to the couch to watch the morning news on TV.. The reason is that if I lay in bed my mind goes back to these early morning events. People wonder why a retired man pops up out of bed at 5:30 AM and goes and watches TV news. I guess it is PTSD. My original thought here is that I think people need to be patient with themselves and accept that an injury to the heart and soul takes time to heal.
Steve March 29, 2018 at 1:45 pm
This is a good article, and I love the visuals, too. I was lost in the maze for a while, and then progressed to the downward slide. The most important thing in my nonprofessional opinion, but one whom has lost a wife of 44 years of marriage, is that you make some progress even if it is extremely slow. I have had a few serious injuries and a couple of surgeries over the years, and sometimes it was over a year to get over a physical injury. My father died in bed (completely unexpected as he was not ill) when I was 17. I know it impacted my life for the next decade or more. My wife died expectantly in bed, but she had been on dialysis for a few years. Sometimes, I ask God if He is trying to drive me crazy. This was kind of cruel. Early in the morning I have to get up from the bed and go to the couch to watch the morning news on TV.. The reason is that if I lay in bed my mind goes back to these early morning events. People wonder why a retired man pops up out of bed at 5:30 AM and goes and watches TV news. I guess it is PTSD. My original thought here is that I think people need to be patient with themselves and accept that an injury to the heart and soul takes time to heal.
JIm Noble December 3, 2017 at 9:09 am
We met when I was 17, she was 16. We were together 50 years exactly – 47 of them married. We evolved together and melded into each other. We had 3 children, 8 grandchildren – the last one she didn’t see – so sad. She died in my arms at home early one morning after caring for her through 18 months of unexpected terminal kidney cancer. She responded well to the treatment, but they don’t tell you about the cachexia and its effects. She just slowly faded away. Three years later and I am now 70 and still having what i call my daily breakdowns. Sometimes they last a few seconds, sometimes minutes but always there are tears and a feeling of deep despair. In my whole life previously I never cried over losing anyone. I have very good family and friends, but they cannot fill the ‘spaces’ in-between . Mealtimes, evenings, bed, driving, shopping etc etc. I live a full life, and am now good at seeming to have fun, but the after joy of events has gone and the sadness is always there. I thought that I needed some therapy so went to my doctor. After filling in an on-line box ticking form 15 pages long, it was decided that I only had a ‘minor upset’. I don’t want to harm myself or anyone else and I function perfectly normally so obviously grief does not compute!
This site has shown me that in fact my behaviour is ‘normal’ and that my way of grieving is just an outpouring of the love that I still have for my wife. Another 50 years together would not have been enough! I miss her so much and always will and I don’t suppose there is a cure for that anyway.
JIm Noble December 3, 2017 at 9:09 am
We met when I was 17, she was 16. We were together 50 years exactly – 47 of them married. We evolved together and melded into each other. We had 3 children, 8 grandchildren – the last one she didn’t see – so sad. She died in my arms at home early one morning after caring for her through 18 months of unexpected terminal kidney cancer. She responded well to the treatment, but they don’t tell you about the cachexia and its effects. She just slowly faded away. Three years later and I am now 70 and still having what i call my daily breakdowns. Sometimes they last a few seconds, sometimes minutes but always there are tears and a feeling of deep despair. In my whole life previously I never cried over losing anyone. I have very good family and friends, but they cannot fill the ‘spaces’ in-between . Mealtimes, evenings, bed, driving, shopping etc etc. I live a full life, and am now good at seeming to have fun, but the after joy of events has gone and the sadness is always there. I thought that I needed some therapy so went to my doctor. After filling in an on-line box ticking form 15 pages long, it was decided that I only had a ‘minor upset’. I don’t want to harm myself or anyone else and I function perfectly normally so obviously grief does not compute!
This site has shown me that in fact my behaviour is ‘normal’ and that my way of grieving is just an outpouring of the love that I still have for my wife. Another 50 years together would not have been enough! I miss her so much and always will and I don’t suppose there is a cure for that anyway.
Martin October 22, 2016 at 4:17 am
I’ve been reading this website for some time since my beloved one died and this is so right, so revealing to me. People use to think that pain, sadness are the worst things can happen. But when you grieve they are so natural as joy when you’re playing with kids. The point is to remember to make sense to your loss and all these negative emotions, thoughts can do that. So let them be or let them go because they are moving, aren’t static. The worst thing can happen is to forget, not to honour the past and at the same time wasn’t consumed by it! Thank you girls!
Jane Mazurek August 10, 2016 at 1:41 pm
My husband died 15 years ago, my older son died 3 years later
and I can still hardly function. My daughter in law described me as broken. And I am. I went to counseling for years and it helped but after having stopped a few months later I am back to grieving.
Jenn Elder August 8, 2016 at 12:01 am
Just fyi and not to diminish the article however: You are not doing anyone a favor by exposing test materials to the public. Its likely copyrighted as well. And yes it is still administered by professionals.
Eleanor August 8, 2016 at 11:20 am
Thanks for your comment. If you’re referring to the inkblot imagine (?), there are many images like this available via creative commons and different stock photo sites. In fact inkblot images are all over the Internet, so I imagine if there are psychotherapists still administering Rorschach tests they are mindful of this fact and account for it in their practice.
Dena May 15, 2016 at 6:33 pm
Your an idiot…don’t tell me how to grieve and what to feel…
Eleanor May 16, 2016 at 2:14 pm
Dena,
I’m confused, where did someone tell you how to grieve or feel?
Eleanor
Jillian May 1, 2016 at 4:04 pm
Once again, thank you for not putting all of us ( grievers) in one box and telling us that there is one way to grieve, one way through it and that we should be over it by now. I love your website.
Alyson April 28, 2016 at 11:41 pm
My first big drop on grief’s rollercoaster came when my parents and I gathered the shiny white shirt, black slacks, and underwear that my sister wore to every orchestra concert to take to the funeral home, who died at the obscene age of eighteen. I saw that my mother was about to take the mary janes that went with her outfit. I had just been dazed up to then, but I suddenly visualized my baby sister buried with her feet stuffed into them, scuffing the cream silk lining in the casket we’d picked, and I just fell apart. I went on a rant about how she hated them I hated them and no one would see them anyway and can’t we please just let her go barefoot. My parents were silent before my father just said that that would be okay and we did.
That was the first time. I’ve fallen apart with rage and sadness at the Starbucks she used to love, at seeing big groups of college students laughing and walking the way she never got to, sometimes a new product or gadget came out and I knew my sister never even got to live in the same WORLD as everyone else with their smartphones and social media. Even sometimes just breathing and feeling the sun and knowing that she is cut off from that forever can still break my heart. Although it’s been nine years, and I’ve gone through lived through so many joys since then, it’s still all there. You’ve helped me much during this recent difficult drop, Elanor.
Michelle April 22, 2016 at 1:25 am
I REALLY needed to read this. Thank you.
Helen April 21, 2016 at 10:51 pm
Hi Patti,I just read your post and my heart goes out to you. I haven’t been through your unique situation but I recently lost my husband,my mother a few years ago and it is a rough road. If u would like to be friends U can get ahold of me. I am 70 years old and a former nurse.
Patty April 21, 2016 at 2:36 pm
This was an excellent post. I lost both my parents recently; Dad on Dec 3, 2015 and Momma Jan 17, 2016…45 days apart. After a year of pure hell leading to their deaths due to their rapid decline (but that is another long, long story). I’m an only child. I want to connect with others who have recently lost both parents at the same time. The stress of all that has happened has caused serious illness for me. I would like to communicate with anyone else who has lost both parents back-to-back but can’t find anyone by searching the web. If you’re reading this and are in the same boat, would you please be willing to respond and share your journey through this horrible nightmare with me? I find this site and these posts most helpful in validating my emotions…that I’m not losing my mind. I’m a 62 y/o very happily married female. My husband is my rock but I don’t think he understands all this completely because he’s much stronger than I can ever hope to be. God Bless you all who are suffering the pain of devasting loss.
Tammy S April 22, 2016 at 9:13 am
Patty,
Oh how I feel your pain. My parents died 4 1/2 months apart. Dad suddenly from a heart attack (revived with hope, then no hope and turning off the ventilator and life support). So hard! Then mom ( who suffered from Parkinson’s symptoms) did well after loosing her care giver and love of 56 years. Mini strokes started and she died after 12 days with hospice. I say she died of a broken heart. I’m not an only child like you, but feel like an orphan at times. I have 3 sisters and 2 brothers, but seem to be having the hardest time with them passing. Since dads death legal work has taken over my life as coexecutor. It doesn’t leave me time to grieve. I’ve made it through 3 holidays and dads birthday. All so hard! And with Mother’s Day approaching my heart sinks. I have a great counselor I found through the hospice we used for mom. I’m so thankful for her. My husband is also my rock and attending my next session. I also have my best friend who’s parents died 5 days apart. I often wondered how she made it through! And through all this I try to move forward and help with my daughters upcoming wedding ( her wedding is 4 days after my dads first year anniversary). These two kiddos have lost four grandparents since they got engaged… Three in the past 7 months. I would be happy to share books I’ve read from my counselor and listen. Walking with others on this journey I feel is great therapy. We all feel the same loss and have that same hole in our hearts. I’m greatful to my other friend who sent me a link to this site!
May God bless you and strengthen you Patty and all who walk this journey.
Karen April 21, 2016 at 10:55 am
Yes, the drawings are as healing for me as your written words. Thank you.
Sylvia April 21, 2016 at 9:44 am
Loved the visuals! And as always, great post and thanks.